Hair Transplant Test Sessions for Scarring Alopecia
Common Errors in Performing 'Test Sesssions'
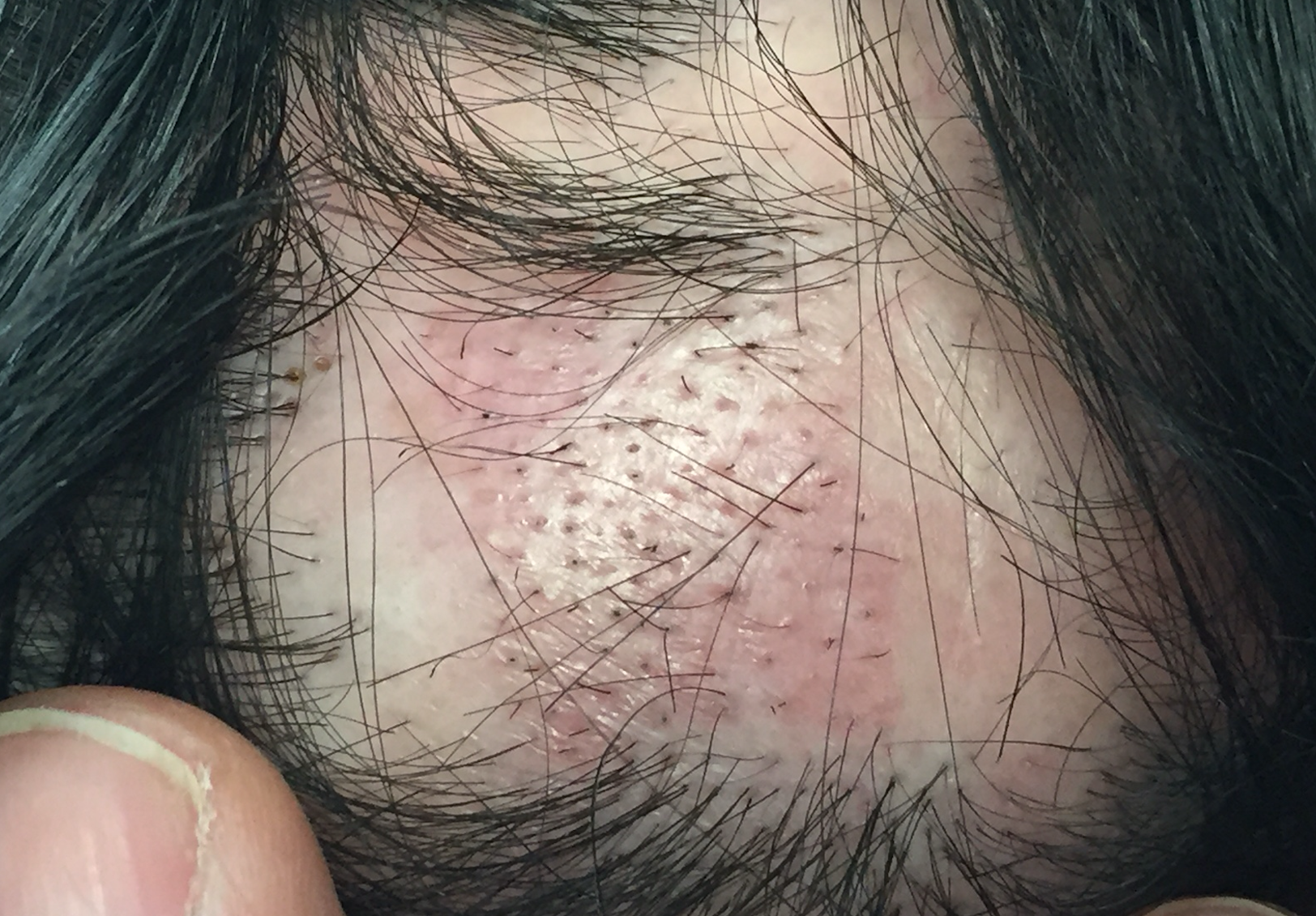
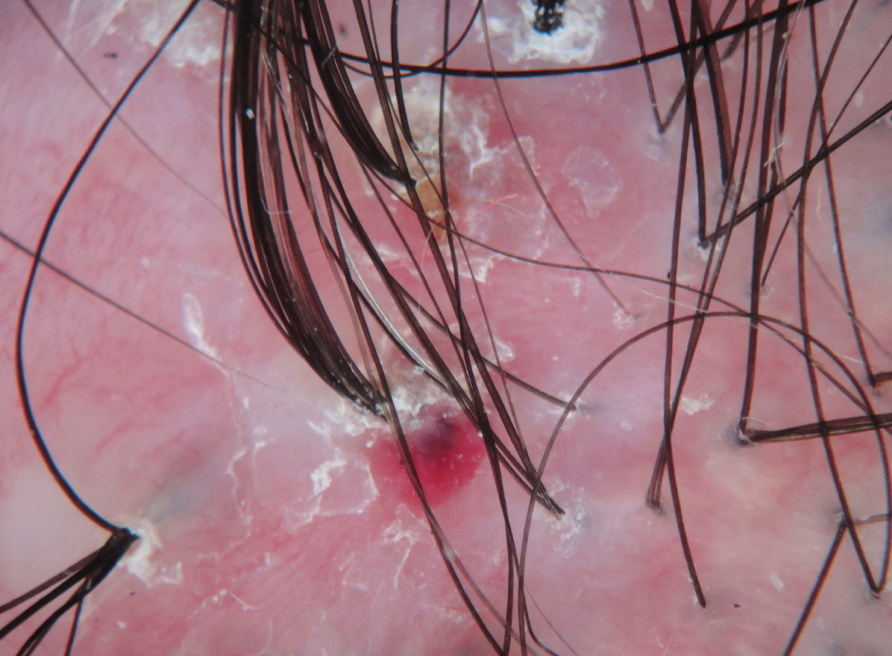
Hair transplants can be an option for patients with scarring alopecia but only if certain criteria are met. First and foremost, the disease should ideally be completely 'inactive' for at least 2 years and the patient should be off all types of immunosuppressive medications. Unless these minimal criteria are met, we can't be sure the scarring alopecia is truly quiet (inactive).
Sometimes a hair transplant “test session” is performed 8-12 month prior to proceeding to the ultimate full hair transplant session. The purpose of the “test session” is to better estimate the chances of success of a larger transplant session. Patients with a successful test session are given the green light to proceed to a full session. Patients with a poor outcome on the tests session may be advised not to proceed with hair restoration in the near future.
I think there is a lot of misunderstanding about how to perform a test grafting session for a patient with scarring alopecia. Below I outline some common errors. But first, let me begin with an analogy.
Hair Transplant Test Sessions: An Analogy
I often use the following analogy when explaining the concepts I believe are important in a hair transplant tes session. As an analogy. imagine yourself offered an exciting job position. 9 months of the year you’ll be travelling to the world's most exotic destinations. The only catch is that 12 weeks of the year, you'll need to be in the arctic circle during the middle of winter. Each day, you’ll need to walk 20 miles through ice and snow collecting various samples. You’ll sleep in a tent each night and you need to carry all your belongings with you.
You are really not sure if you’ll be able to withstand the cold and all your friends think you’ll crazy for thinking about accepting the position as they think you are far to soft of a person to withstand the cold and extremes of the artic circles. To test whether you can really survive an article winter, you decide to make a “test visit” for 1 month to see if you’ll really like living there or not. You figure if you can survive 4 weeks, 12 weeks should not be so bad.
As you are deciding when to go, a friend advises you to go in the summer since she’s heard it’s lovely in the summer. Another friend advises you to go in the winter but stay at some luxury accommodations he’s heard good things about.
In my opinion, neither pieces of advise from these friends is really ideal for a ‘test visit.’ To challenge yourself to see if you are really going to withstand the arctic winter, you need to visit in the winter - and you need to stay in lodging that best represents how you’ll live if you do decide to move. That lodging is, of course, a tent. It’s reasonable to bring two blankets with you and a few more warm belongings that most people who live in the area normally use – because let’s face it – the whole experience is completely new to you.
The same is true with a transplant test session. The whole experience of moving from a warm, richly vascularized area into a scarred, poorly vascularized area is a big challenge for a little hair follicle. During a 'test session, I believe one needs to challenge these little hairs and see if they really can make it. One needs to make the scalp suitable to growing but not too perfect and luxurious that it falsely misrepresents the challenges that will ultimately be present if a real transplant is performed. Newly transplanted hairs are not really used to growing in scar tissue and not used to growing in between the little bits of inflammation that are often there – so it’s reasonable to help them out a bit. But my opinion is that a test session should truly be a test session. The hairs need to be tested !
COMMON ERRORS IN "TEST SESSIONS"
1. Excessive topical corticosteroids and immunosuppressives are used
A test session is really all about testing whether hairs can withstand the challenges of growing in less than ideal conditions. The new grafts need to grow in scarred scalp tissue that may lack ideal blood supply. The skin itself may be too thick or too thin.
As part of the test session, I believe on should use minimal corticosteroids (and minimal other immunosuppressives if at all possible). It's still okay to use them but just not excessively. I typically recommend steroids a few times per week before the test transplant with steroids stopped one month before. Steroids are started again 1 month after the test session but only twice weekly for two months and then once weekly thereafter. A mid potency topical steroid should be sufficient.
One needs to challenge these little hairs and see if they really can make it. One needs to make the scalp suitable to growing but not too perfect and luxurious that it falsely misrepresents the challenges that will ultimately be present if a real transplant is performed. The analogy is similar to the arctic circle analogy I used above.
2. The grafts are spaced too far apart
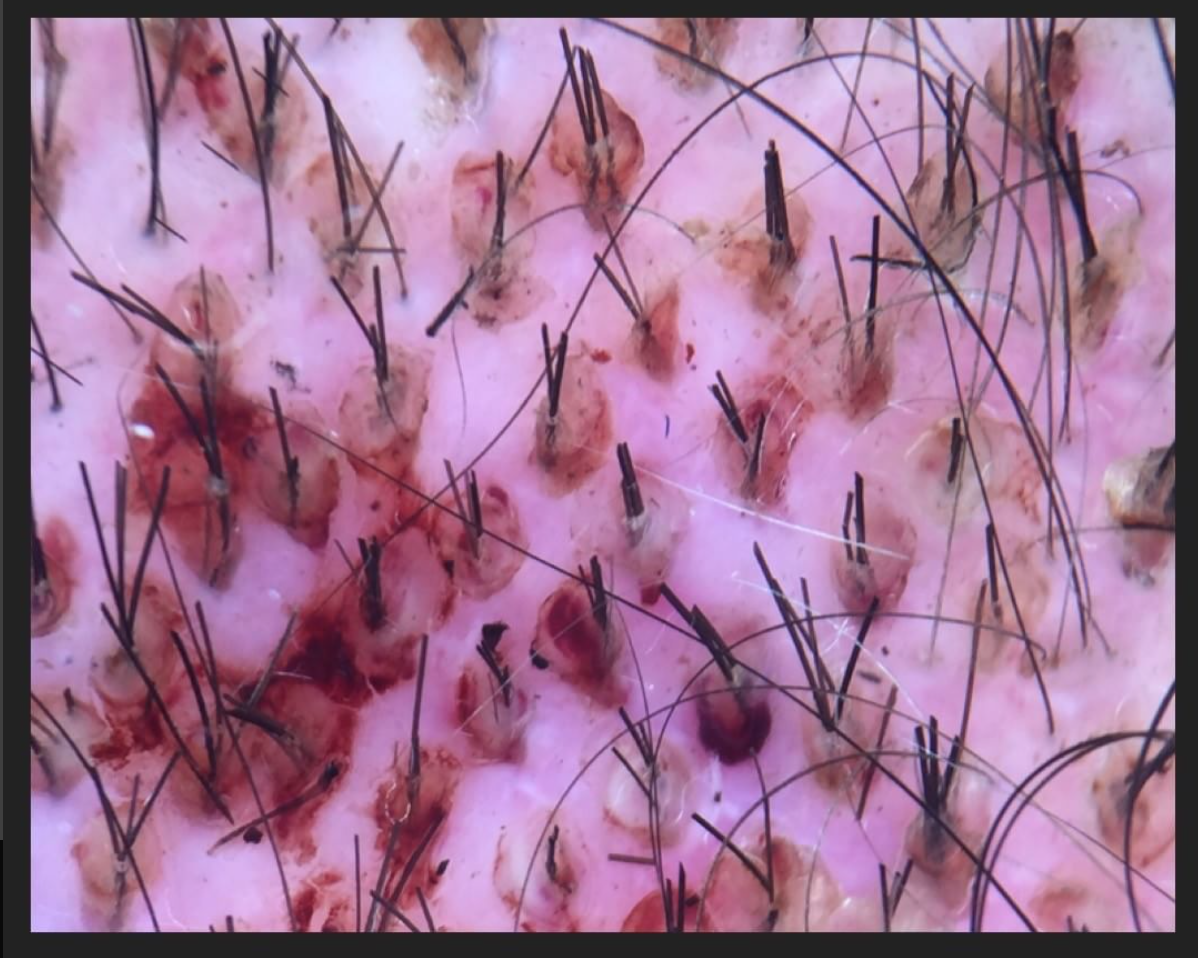
Ideally, 100-200 grafts should be put in an area at a density of 25-30 follicular units per cm2 and this area carefully followed over time. The problem with placing grafts at a lesser density is that it does not adequately ‘stress’ the hair follicles during the test session. When it comes to growing in scar tissue, it’s easier for hairs to grow when they are far apart rather than close together. My view is that during a ‘test session’we need to understand how the hair follicles survive under realistic situations. If the patient ultimately proceed to a full hair transplant session, follicle are going to be transplanted at a density of 20-25 follicular units per square cm AT MINIMUM and so a test session should slightly exceed this. We need to test the follicles!
3. Too many grafts are put in
I don’t recommend that test sessions be done with more than 200 grafts and 150 is often ideal. The problem with doing more than 200 is that it become difficult to count the grafts.
I have seen patients who come to see me after have 500-800 grafts ‘peppered’ into the front of the scalp or ‘peppered’ into the crown. Instead of putting 100-150 follicles in to an area the size of a golf ball, 500-800 grafts get put into an area the size of a large melon or small dinner plate. It is easy to count 100-200 grafts (1, 2, 3, 4…) but more difficult to count 500. When it comes to hari transplant test session, I believe we need accurate survival numbers. Knowing that 90% survived is very different than knowing 54 % survived. Knowing that the survival 'seemed ok' is very different than knowing that the survival was 'excellent.'
4. The grafts are put into an area already containing hair follicles
In my opinion, a test session should be performed in an area with as few hairs as possible, ideally with no hair. Sometimes this is not possible, but if it is –this should be followed. This makes it easier to document “before and after”photographs, count hairs and document clearly the survival of grafts.
The problem with putting in 500-1000 grafts in area area that already has hair, is that it becomes impossible to really get a sense of the proportion of grafts surviving at a time 9-12 months post op. I saw a patient recently who had 500 grafts placed into his crown. The test session was performed in an area that was thinning but not bald. It was impossible to really get a sense of how many grafts survived, despite the fact that the surgeon estimated survival waspretty good. Photos suggested there were no changes to the density and the patient felt it had worsened! Objective measurements are what is needed in these test session.
5. The grafts are put in an area that is not representative of the actual scalp to be transplanted
Hair follicles need to be placed in an area that is representative of the average quality of the skin of the scalp, and possibly even in an area that represents slightly poorer than average quality. If much of the scalp contain thicker areas of scar tissue, this is not unreasonable to perform the test session in there. If most of the scalp is thick pale, poorly vascularized tissue and only a small portion of the scalp is pink normal appearing skin, it is misrepresentative to perform the test tession in the pink, normal appearing area.
Returning to the analogy above, it is unreasonable (in my opinion) for a person undergoing a test visit to the article circle to stay in a luxury accommodation during the visit when the whole purpose of the visit is to see if one can really withstand the extremes of living in the article circle. In the same way, it is unreasonable to make the test session a wonderful opportunity for hair growth.
A test session should represent a true... test!
This article was written by Dr. Jeff Donovan, a Canadian and US board certified dermatologist specializing exclusively in hair loss.