Hair Transplants for Folliculitis Decalvans: Is it even possible?
FOLLICULITIS DECALVANS
HAIR TRANSPLANT CANDIDACY CRITERIA
The criteria we use in our clinic for evaluating folliculitis decalvans candidacy are among the most strict of all the scarring alopecia criteria. Hair transplants for folliculitis decalvans can be very challenging. Chances of success are low although successes to occur. In order to be a candidate for hair transplant surgery, ALL FIVE of the following criteria MUST be met in a patient with folliculitis decalvans:
1. The PATIENT should be off all hair-related medications.
Ideally the patient should be off all topical, oral and injection medications to truly know that the disease is "burned out (burnt out)". However, in some RARE cases, it may be possible to perform a transplant in someone using medications AND who meets criteria 2, 3 and 4 below. This should only be done on a case by case basis and in rare circumstances. It is a 'last resort' in a well-informed patient.
2. The PATIENT must not report symptoms related to the FD in the past 24 months.
The patient must have no significant itching, burning or pain and no bleeding. One must always keep in mind that the absence of symptoms does not prove the disease is quiet. Even the periodic development of itching or burning from time to time could indicate the disease has triggers that cause a flare and that the patient is not a candidate for surgery. The patient who dabs a bit of clobetasol now and then on the scalp to control a bit of itching may also have disease that is not completely quiet. The patient with itching every now and then is also a worry.
3. The PHYSICIAN must make note of no clinical evidence of active disease in the past 24 months.
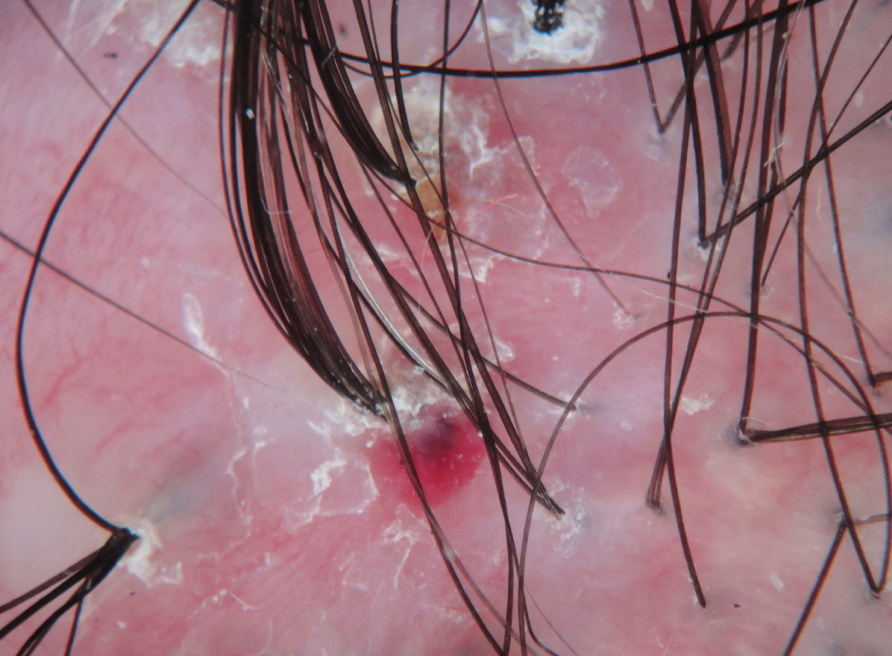
There must be no scalp clinical evidence of active FD such as perifollicular erythema, pustules, crusting, perifollicular scale (follicular hyperkeratosis). This assessment is best done with a patient who has not washed his or her hair for 48 hours.
The most important clinical features in our opinion are SCALP CRUSTING and REDNESS AROUND THE HAIRS. Some scalp redness may be persistent in patients with scarring alopecia even when the disease is quiet. Therefore scalp redness alone does not necessarily equate to a concerning finding. Perifollicular redness (redness around the hairs) however is more concerning for disease activity. In addition, the pull test must be completely negative for anagen hairs and less than 4 for telogen hairs. A positive pull test for anagen hairs indicates an active scarring alopecia regardless of any other criteria.
4. Both the PATIENT and PHYSICIAN must demonstrate no evidence of ongoing hair loss over the past 24 months.
There must be no further hair loss over a period of 24 months of monitoring off the previous hair loss treatment medications. This general includes the patient's perceptions and physician's perception that there has been no further loss, physician's measurements showing no changes in the areas of hair loss, as well as serial photographs every 6-12 months showing no changes.
5. The patient must have sufficient donor hair for the transplant.
Not all patients with FD have sufficient donor hair even if their disease has become quiet.
In situations where there is concern that the FD may be active or concern that the surgery may not be a success, strong consideration should be given to performing a 'test session' of 50-100 grafts and observing their survival over a period of 6-9 months. Less than 40 % uptake would intake a contraindication, although ideally one would hope for survival of more than 70% of the grafts.
For Further Reading
Lichen Planopilaris Transplant Candidacy
Frontal Fibrosing Alopecia Transplant Candidacy
Trichotillomania Candidacy: Can a patient with trichotillomania have a hair transplant?
This article was written by Dr. Jeff Donovan, a Canadian and US board certified dermatologist specializing exclusively in hair loss.